Administration
According to the IRS good records are used to monitor the progress of your business. Corporate records can show whether your business is improving, which services you may want to add, or what changes to make. Excellent record– keeping can increase the likelihood of business success. And when any of your Credentialed federal, state or commercial health insurance representatives show up on-site, you are 100% prepared by QPI and through Lavear for a review of all operational documents, licenses, accreditations, and credentials.
Corporate Structure Management
We take federal regulations, accreditation standards, state statutes, local laws and payer/ insurance requirements and apply them, electronically, to our clients’ organizations’ administration. Our dedicated Program Managers work with our clients and organizations one-on-one to ensure compliance administration and standards implementation. Requirements are satisfied in personnel files, operational documents, policies and procedures and in daily quality assurance activities—all housed in Lavear.
Our series of checks and balances ensures that the organization runs smoothly, efficiently and compliantly.
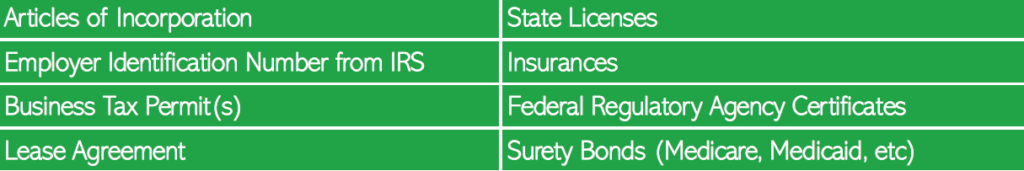
Credentialing for Organizations
Licensing is now more than just registration and maintenance with providers’/ organizations’ home state. In the world of telehealth and nationwide networks, many providers are also becoming licensed in other states. QPI assists in licensing and credentialing providers/ organizations. We work with you to strategize growth into your home state and surrounding states, and assist in applying, obtaining, and renewing appropriate licensing in each state.

Credentialing doesn’t stop at licensing. Often, healthcare providers spend time and money applying to become enrolled with Health Insurance Networks as in-network providers with federal, state, and commercial health insurance plans when seeking reimbursement from care, treatment, or services that have been delivered to patients.
Over time, the relationships that we have worked hard to establish with our patients’ insurers are mistaken with a “set it and forget it” mindset. Provider to insurance relationships are not stagnant. Patient care is not stagnant. Patients’ insurance premiums and Providers’ reimbursements are also not stagnant.
QPI’s Credentialing Team ensures that all credentials are maintained and renewed. We work with Providers to remind leadership teams when to renegotiate contracts.
QPI will also work with Providers to strategize growth based on your specialty, service areas and patient needs. We believe that advising patients “we don’t accept your insurance” is unacceptable in most circumstances.
Our team works with Providers to devise a game plan to apply and reapply to closed networks in order to maximize your patient reach, ultimately increasing revenue.
Growth, increased patient outreach, and enrollment with health insurance plans is great, but we can’t forget the root of it all—compliance administration and standards implementation, both of which tie back into QPI’s HARP Light Technology.
Accreditation Organization Management (If Applicable)
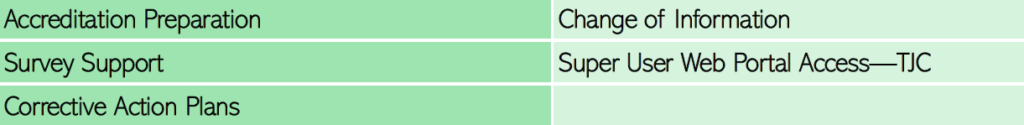
Formal audits may be conducted by Accreditation Organizations for your organization’s participation in any federal, state, or commercial health insurance program. QPI is here to assist healthcare providers/ organizations in becoming initially accredited, reaccredited, and in reporting changes within the organization to the accreditation organization. Through Lavear, QPI offers a “Report On-Site Surveyor” feature. This allows providers immediate, direct, and uninterrupted access to QPI’s Program Managers for assistance in producing requested documentation and other support during survey.
Additionally, QPI will work with organizations to respond to any deficient or cited standards during survey that require any additional corrective action plan or clarification after survey.
Standards Implementation
Organizational credentialing and licensing are driven by Providers’ delivery of quality care. At times, federal and state health insurance plans may require Providers to become accredited. Healthcare accreditation is an independent evaluation from a CMS pre-approved third-party to confirm Providers’ implementation and formal demonstration of industry standards.
Among standards implementation, many health insurance requirements include validation of policies and procedures. What is your written word? And is it standardized for implementation within your organization, unilaterally?
HARP Light Technology is essentially a SIM (Standards Implementation Methodology) Technology. Our process is simple. Together, we define your goals, measure aspects of your processes, analyze data, suggest methods to improve your processes and discuss ways to control future performance.

HARP Light Technology is essentially a SIM (Standards Implementation Methodology) Technology. Our process is simple. Together, we define your goals, measure aspects of your processes, analyze data, suggest methods to improve your processes and discuss ways to control future performance.
QPI works with healthcare organizations to implement Codes for Federal Regulations, Conditions of Participation, Accreditation Standards, State Statutes, Quality Measures and more, in Lavear. Our Program Managers create tasks and audit supporting documentation to assist Providers in formally demonstrating standards implementation for federal, state and commercial health insurances.







